Learn more about Haemorrhoids
Did you know that haemorrhoids are so common, that they will cause symptoms in at least 1 in 3 people? Read on for more, and remember that you are not alone!
Haemorrhoids (or ‘piles’) are the enlargement of a small network of blood vessels in the anal canal. They are very common – affecting between 25-50% of the population. They do have a normal function, and help to occupy space in the anal canal, and contribute to anal tone – this helps prevent soiling, leakage, and the involuntary loss of wind.
Haemorrhoids can lose their attachement to the wall of the anal canal, allowing them to slide, enlarge and prolapse. As haemorrhoids enlarge, they become fragile and can cause bleeding – this is usually small volume, bright red, and fresh blood on the toilet paper, in the bowl, or on the outside of the stool. Occasionally, blood will leak into the underpants, particularly with passing wind. Bleeding from haemorrhoids can be major, but this is less common. Bleeding after anal sex may be due to trauma or tears, or aggravation of underlying haemorrhoids.
Whilst haemorrhoids are benign and rarely dangerous, it is important to exclude more worrying causes of rectal bleeding. This includes rectal polyps or rectal cancer, and unfortunately in young people, rectal cancer is increasing in incidence. We cannot presume that bleeding is due to haemorrhoids. Bleeding is not normal, and you should see your doctor – don’t die of embarassment.
Haemorrhoids can also prolapse to the outside, with defecation, passing wind or even physical activities. These can irritated, uncomfortable, and they can cause soiling, mucous and ‘skid marks’. Prolapsed haemorrhoids can make cleaning difficult, and the combination of leakage and difficulty with cleaning can cause itch and irritation of the skin around the anus. If haemorrhoids get really stuck on the outside, they can become very swollen and painful – this is called “acute thrombosed prolapsed haemorrhoids”.
Unless they do become stuck, haemorrhoids aren’t typically painful – and this is a common misconception. Pain associated with defecation is not usually haemorrhoids, and we need to consider other diagnoses such as an anal fissure, fistula, infection or cancer.
There are multiple options for treating haemorrhoids – and there are even painless options!
Dr Morris is an enthusiast for avoiding painful haemorrhoid treatments where possible, and has a range of minimally invasive options that will be discussed if suitable, for you. It is important that your surgeon considers your function, and your goals, for example, if bottoming is important to you, then this should be considered, addressed, and please feel comfortable raising it – Dr Morris talks about this all day!
Please see some of these options below, and in the “Procedures” tab, but your possible options will be carefully discussed in your consultation.
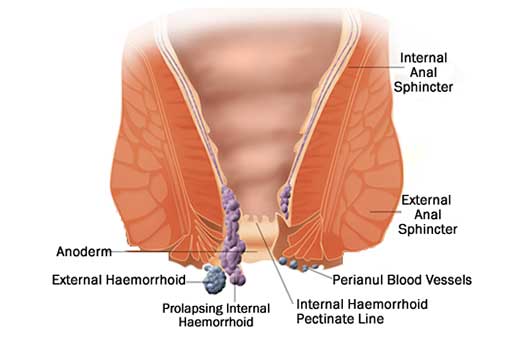
The treatment for haemorrhoids depends on the severity of symptoms and the size or grade of the haemorrhoids. It also depends on you, your goals and wishes, and how you use your bottom.
In minor degrees of haemorrhoids, treatment is often through changes in behavious. It is important to avoid constipation and aid the passage of stool. This is done by measures such as increasing water intake, exercise, dietary fibre in the form of increased fruit and vegetables. A fibre supplement has been shown to reduce bleeding and symptoms by 50%. A fibre supplement eg. psyllium husk, is easily obtainable and palatable, and should be the first measure to reduce your symptoms.
A simple rule of thumb however, is not to avoid seeking treatment. By all means institute these basic measures, but should your symptoms persist for more than 2 or 3 weeks. Then please seek attention. Don’t die of embarassment.
For haemorrhoids requiring intervention, there are options for treatment. Your haemorrhoids may be the tip of an iceberg of a defecatory problem, thus assessment needs to be tailored to you.
If we think about haemorrhoids as a package of blood vessels, a simple intervention involves reducing the blood supplying them. This allows them to shrink and contract. Options include rubber band ligation, haemorrhoid energy therapy, haemorrhoid artery ligation, and injection sclerotherapy.
Rubber band ligation is still widely performed, and effective for early grade haemorrhoids. In this technique, a tight band constricts the blood supply and excess tissue – likely docking a sheeps tail – and allowing it to die and fall off. Unfortunately this procedure is often painful, irritating, and has a risk of bleeding when the band falls off in 7-10 days.
A newer technique called Haemorrhoid Energy Therapy (HET) is a painless option for many people, and has largely replaced the use of rubber band ligation Dr Morris’ practice. It works by utilising the application of a low heat to coagulate the blood vessel supplying the haemorrhoid, allowing the haemorrhoids to shrink and contract. This avoids a painful band, and avoids tissue damage and ulcers – thus reducing the risk of bleeding, and improving comfort.
Either of these techniques can easily be coupled with colonoscopy, so that a colonoscopy to investigate bleeding can have haemorrhoids treated at the same time. This requires less time off work, and almost no restriction of activities after treatment.
Higher grade haemorrhoids may require formal surgery, and Dr Morris discuss the options with you, but they may include the following:
Haemorrhoidal arterial ligation and rectoanal repair (HAL-RAR) is a well tolerated (and often painless) technique, where an ultrasound is used to guide a stitch to tie off the haemorrhoidal artery. The prolapsing component of the haemorrhoid is then tightened, a little like a ‘facelift of the anus’. This is repeated all the way around the anal canal, and is a common option particularly for women after childbirth, where continence is a concern, and where anal sex is important rendering possible side effects of alternative operations less acceptable.
An excisional haemorrhoidectomy is reserved for the largest haemorrhoids, and the benefits and drawbacks of this operation will be discussed. This is traditionally a very painful operation, but remains very effective, and sometimes a necessary option.
Dr Morris is trained in stapled haemorrhoidectomy, but has chosen not to offer this procedure given the particular risks of this procedure. Whilst other surgeons may offer this procedure, Dr Morris has decided that the risks of possible chronic pain, rectovaginal fistula, rectal dysfunction and infection are not worth the risks for his patients. For patients in whom anal sex is important, the presence of a potentially sharp staple line is of particular concern and should be avoided, with case reports in the literature reporting possible penile or condom damage with anal sex.
Dr Morris will assess your symptoms, and perform a careful examination to allow a tailored discussion to approach your haemorrhoid symptoms together.
Please consider persistent rectal bleeding as a symptom requiring urgent assessment. There are many causes of rectal bleeding, and we can very quickly delineate the precise cause. Please consider this important symptom a potential warning sign, and see your GP and/or your Colorectal Surgeon. A CSSANZ Accredited Colorectal Surgeon can be found at https://cssanz.org/ and “find a surgeon”.